
From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:


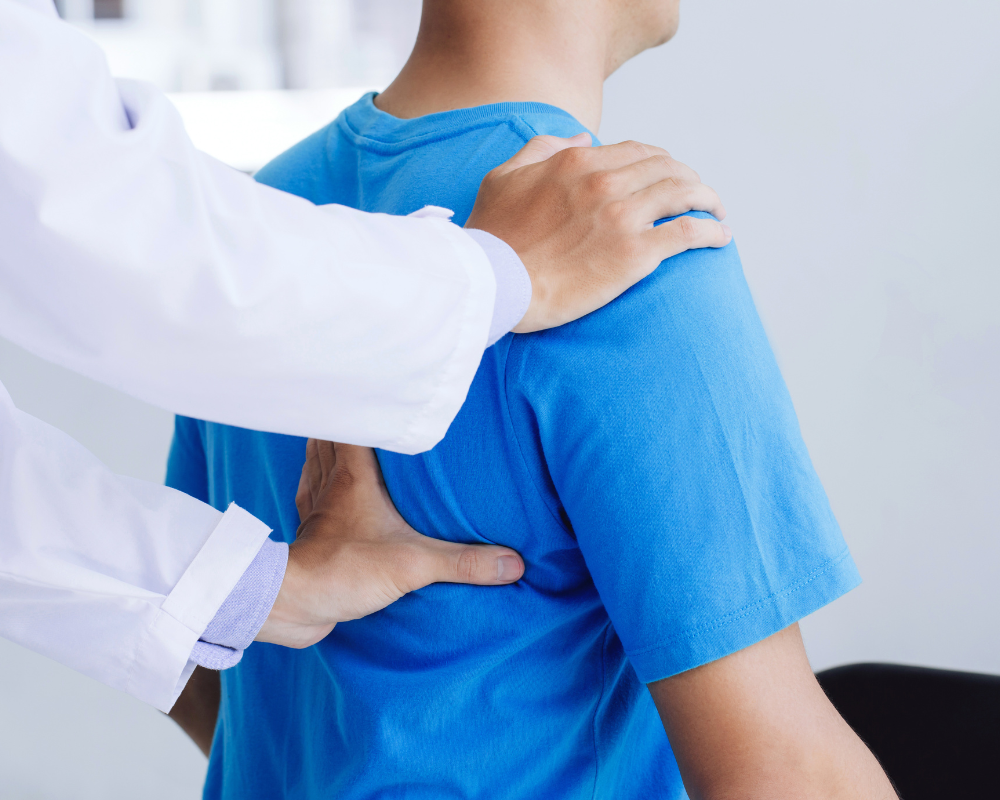
Physiatry, also known as physical medicine and rehabilitation (PM&R), is a medical specialty focused on restoring function, improving movement, reducing pain, and helping patients return to daily life without surgery whenever possible.
Physiatrists diagnose and treat conditions affecting the spine, nerves, muscles, joints, and supporting soft tissues.
In spine care, this includes conditions such as sciatica, cervical radiculopathy, lumbar disc herniation, spinal stenosis, degenerative disc disease, and low back pain.
The goal is not just symptom relief—it’s understanding why symptoms are happening, how they affect function, and which non-surgical strategies will lead to lasting improvement.
Key Point:
Physiatry is especially valuable when the right answer isn’t obvious. Many patients don’t need surgery—but they do need a structured plan and clear direction.
Most patients benefit from:
Because the majority of spine conditions do not require surgery, physiatry plays a central role in guiding care.
Typical Treatment Pathway:
Diagnosis → Rehabilitation & Medication → Image-Guided Injections → Surgical Evaluation (if needed)
This coordinated approach ensures patients don’t get stuck in endless treatment cycles without direction—and don’t undergo surgery prematurely.
One of the most important roles of physiatry is identifying the true source of pain and dysfunction.
Imaging findings alone don’t always explain symptoms. Dr. Paul relies on physiatry to bridge that gap between imaging and real-world function.
Diagnostic Precision
Aligning symptoms, physical exam findings, and imaging
Functional Assessment
Evaluating strength, mobility, posture, and activity limitations
Non-Surgical Treatment Planning
Coordinating therapy, medications, and targeted procedures
Long-Term Management
Adjusting care over time and recognizing when escalation is needed
This approach helps avoid both unnecessary procedures and delays in appropriate treatment.

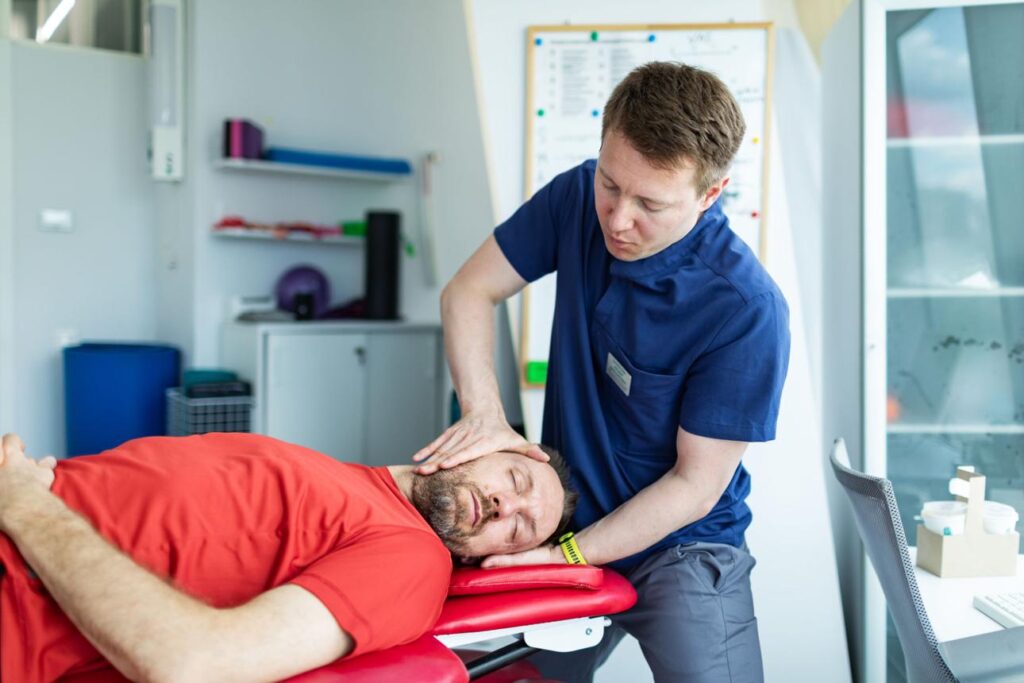
Short-term use of anti-inflammatory or nerve-related medications can help reduce pain and allow patients to actively participate in recovery.
Structured physical therapy is a cornerstone of treatment and may include:
Exercise-based care remains one of the most effective non-surgical treatments for spine conditions.
Targeted injections—such as epidural steroid injections—may:
Long-term recovery often depends on:
Clinical Philosophy:
Dr. Paul’s approach is not focused on temporary pain relief—it’s focused on restoring function and preventing recurrence.
Physiatry is highly effective for:
Multidisciplinary, exercise-based care is strongly supported in the literature for improving both pain and function.
Non-surgical treatment should not become endless without results.
Dr. Paul emphasizes timely reassessment when:
At that point, the next step may involve targeted procedures such as:
When appropriate, these procedures may be performed using outpatient spine surgery techniques, allowing patients to return home the same day with less disruption to recovery.
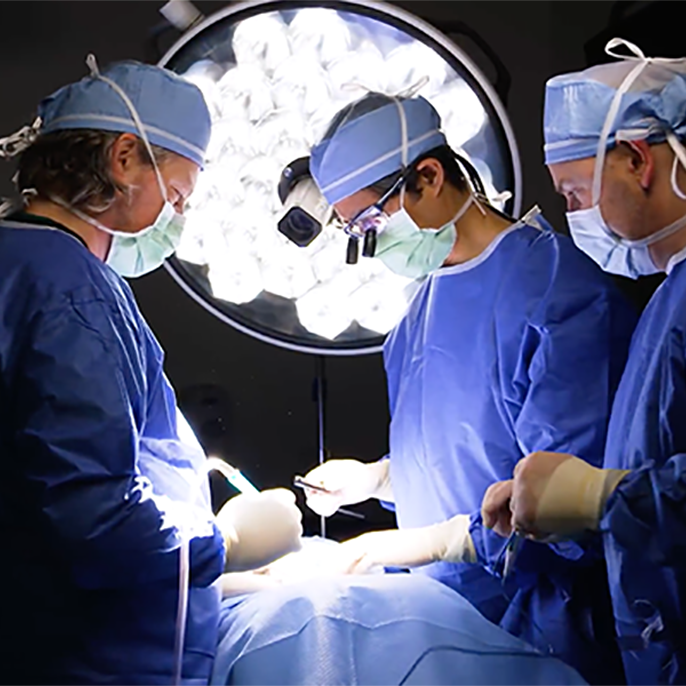

A physiatrist is a physician trained in physical medicine and rehabilitation (PM&R). In spine care, physiatrists focus on diagnosis, pain reduction, functional recovery, rehabilitation planning, and non-surgical treatment. Dr. Paul often works with physiatrists to ensure patients receive a comprehensive, function-focused evaluation before considering more advanced treatments.
Not always, but many patients benefit from a physiatry evaluation because it helps clarify whether non-surgical care is likely to work and whether surgery is actually necessary at that point. Dr. Paul often incorporates physiatry as part of a coordinated care plan to ensure the right treatment path is chosen early.
Yes. Physiatry is often very helpful for sciatica and lumbar disc herniation, especially when the goal is to reduce inflammation, improve mobility, and avoid surgery when safe and reasonable. Many patients improve with structured non-surgical care, while others may later transition to procedures—including outpatient spine surgery—if symptoms persist.
Treatment may include physical therapy, medication management, activity modification, patient education, and targeted injections such as epidural steroid injections. These treatments are often used together to reduce pain, improve function, and support long-term recovery.
There is overlap, but physiatry typically places a stronger emphasis on function, movement, rehabilitation, and long-term recovery rather than symptom suppression alone. Dr. Paul integrates this approach to ensure patients are not only feeling better, but actually improving in strength, mobility, and daily function.
If symptoms persist despite a structured treatment plan, or if weakness, numbness, or balance problems worsen, it may be time for more advanced imaging review or surgical evaluation. In these cases, Dr. Paul helps determine whether continued non-surgical care is appropriate or if a more definitive solution—such as outpatient spine surgery—should be considered.
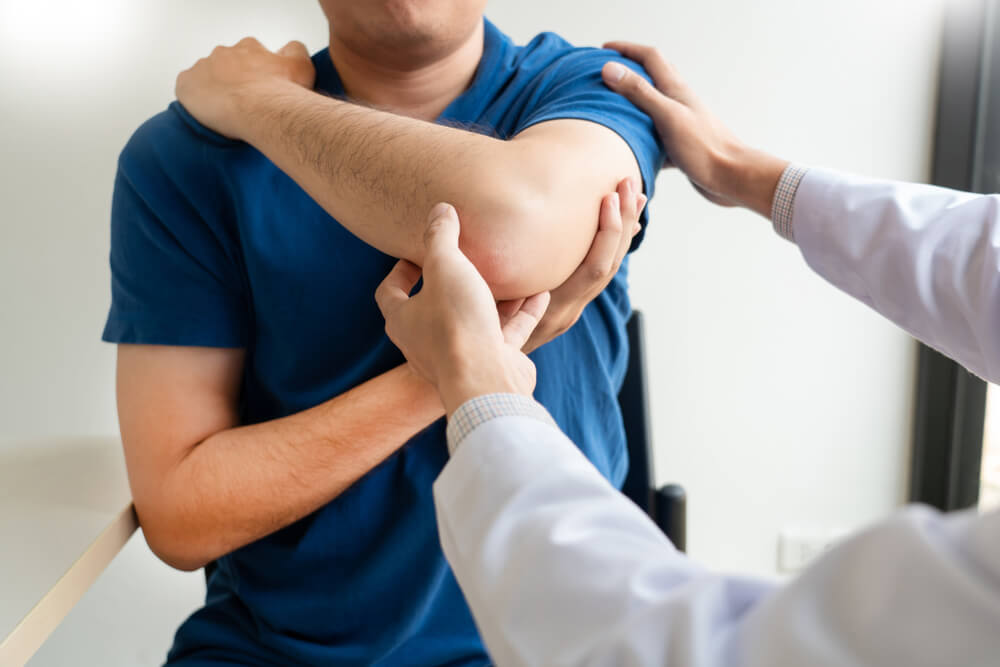
Physiatry plays a critical role in modern spine care by helping patients avoid unnecessary surgery while ensuring they don’t delay needed treatment.
Dr. Paul’s approach combines:
The result is a care pathway that prioritizes function, recovery, and long-term outcomes—whether that involves non-surgical treatment or outpatient spine surgery when appropriate.
References

