
From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

Sciatica refers to pain that travels along the path of the sciatic nerve, typically starting in the lower back or buttock and radiating down the leg. It is one of the most common causes of leg pain and can range from mild discomfort to more severe nerve-related symptoms.
Dr. Paul focuses on identifying the exact cause of nerve irritation before recommending treatment. While sciatica can feel intense, most cases improve with structured non-surgical care that reduces inflammation and restores normal movement.

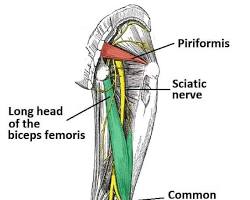
Sciatica is not a condition by itself, but rather a symptom caused by irritation or compression of one or more nerve roots in the lower spine. These nerves come together to form the sciatic nerve, which runs from the lower back down through the leg.
When a nerve root becomes inflamed or compressed, pain can travel along the entire nerve pathway. This is why symptoms are often felt in the buttock, thigh, calf, or even the foot rather than just the lower back.
Common underlying causes include lumbar disc herniation, spinal stenosis, spondylolisthesis, and degenerative changes in the spine.
Common symptoms include:
The most common cause is a lumbar disc herniation pressing on a nerve root. Other causes include narrowing of the spinal canal, joint degeneration, or instability in the spine. In some cases, irritation can also occur outside the spine, such as with piriformis syndrome.
Diagnosis begins with a clinical evaluation focused on identifying nerve involvement and determining the underlying cause. A physical exam often includes specific tests, such as the straight leg raise, which can reproduce symptoms when a nerve is irritated.
Neurological testing helps assess strength, reflexes, and sensation to determine which nerve root may be affected. MRI is typically reserved for cases where symptoms persist, worsen, or involve weakness, as it provides a detailed view of nerve compression and spinal structures.
The key is to match imaging findings with symptoms, ensuring that treatment targets the true source of pain.
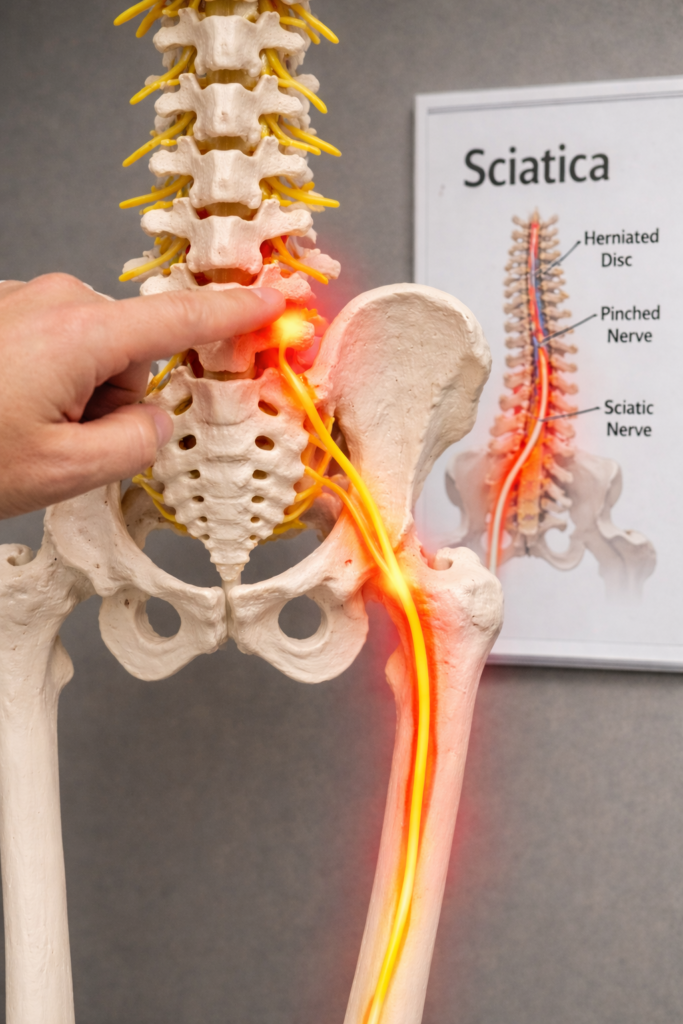

The majority of sciatica cases improve without surgery, with most patients recovering within several weeks to a few months.
Treatment focuses on reducing inflammation around the nerve and restoring normal movement. Physical therapy plays a central role, helping improve flexibility, strengthen supporting muscles, and reduce mechanical stress on the spine. Medications may be used to manage pain and nerve irritation, while targeted injections can provide temporary relief in more persistent cases.
Daily habits also matter. Avoiding prolonged sitting, maintaining good posture, and staying active can significantly improve recovery and reduce recurrence.
Surgery is considered when symptoms do not improve with non-surgical care or when neurological deficits develop. This may include progressive weakness, significant functional limitation, or imaging findings that clearly show nerve compression matching symptoms.
In these cases, procedures are designed to relieve pressure on the affected nerve while preserving as much normal structure as possible. Most commonly, this involves removing the portion of disc or tissue causing the compression.

Sciatica is pain that travels from the lower back or buttock down the leg because one of the lumbar or sacral nerve roots is irritated. It is a symptom pattern, not a single diagnosis by itself.
The most common causes are lumbar disc herniation, spinal stenosis, degenerative changes, or spondylolisthesis. Less commonly, symptoms similar to sciatica can come from piriformis syndrome or other problems outside the spine.
Patients often describe sharp, burning, electrical, or shooting pain down the leg. Tingling, numbness, or a sense of leg heaviness can happen too, especially with sitting, bending, coughing, or prolonged driving.
Many people improve within 6 to 12 weeks, especially when they stay active and follow a structured non-surgical plan. Some improve faster, while others take longer depending on how irritated the nerve is.
In many cases, yes. Gentle walking can reduce stiffness and support recovery better than prolonged rest. The key is pacing activity rather than avoiding movement altogether unless a clinician advises otherwise.
Urgent evaluation is needed if there is progressive weakness, foot drop, severe numbness in the groin or saddle area, or loss of bladder or bowel control. Those symptoms may suggest a more serious neurologic problem.
Common treatments include physical therapy, walking, posture and lifting adjustments, anti-inflammatory medication, nerve pain medication when needed, and sometimes epidural steroid injections to reduce inflammation around the nerve.
Surgery is considered when severe leg pain remains disabling despite good conservative care, or when there is clear and progressive neurologic loss such as worsening weakness or foot drop.
References
1. Stafford MA et al. Sciatica: Diagnosis and Management. BMJ. 2007.
2. Dydyk AM et al. Sciatica. StatPearls [Internet]. NCBI Bookshelf; updated 2024.
3. Weinstein JN et al. Surgical vs Non-Operative Treatment for Lumbar Disc Herniation:
SPORT Trial. N Engl J Med. 2006.
4. Kreiner DS et al. NASS Guidelines for Lumbar Radiculopathy and Disc Herniation.
North American Spine Society; 2022.
5. National Spine Health Foundation. Educational Resources on Sciatica and Nerve Pain.
2024.
6. Peul, W. C., et al. (2007). Surgery versus prolonged conservative treatment for sciatica. New England Journal of Medicine, 356(22), 2245–2256

