
From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

Lumbar microdiscectomy is one of the most established procedures in spine care. It is typically used to treat a lumbar disc herniation that is pressing on a nerve and causing sciatica, especially when leg pain, numbness, or weakness continue despite appropriate non-surgical treatment.
Dr. Paul performs microdiscectomy using a precise, tissue-sparing technique designed to remove the portion of the disc compressing the nerve while minimizing disruption to surrounding structures. When symptoms clearly match the diagnosis, this procedure provides reliable and targeted relief.

Microdiscectomy is most effective when symptoms are clearly caused by a lumbar disc herniation that matches the patient’s exam and imaging findings.
The best outcomes are typically seen in patients with leg-dominant pain, persistent symptoms despite non-surgical care, and neurologic findings such as numbness or weakness that align with imaging.
Clinical guidelines from the North American Spine Society support discectomy as a more effective option than continued medical or interventional care when symptoms warrant surgery. Evidence also suggests that surgery performed within 6 months of symptom onset may be associated with better outcomes in appropriately selected patients.
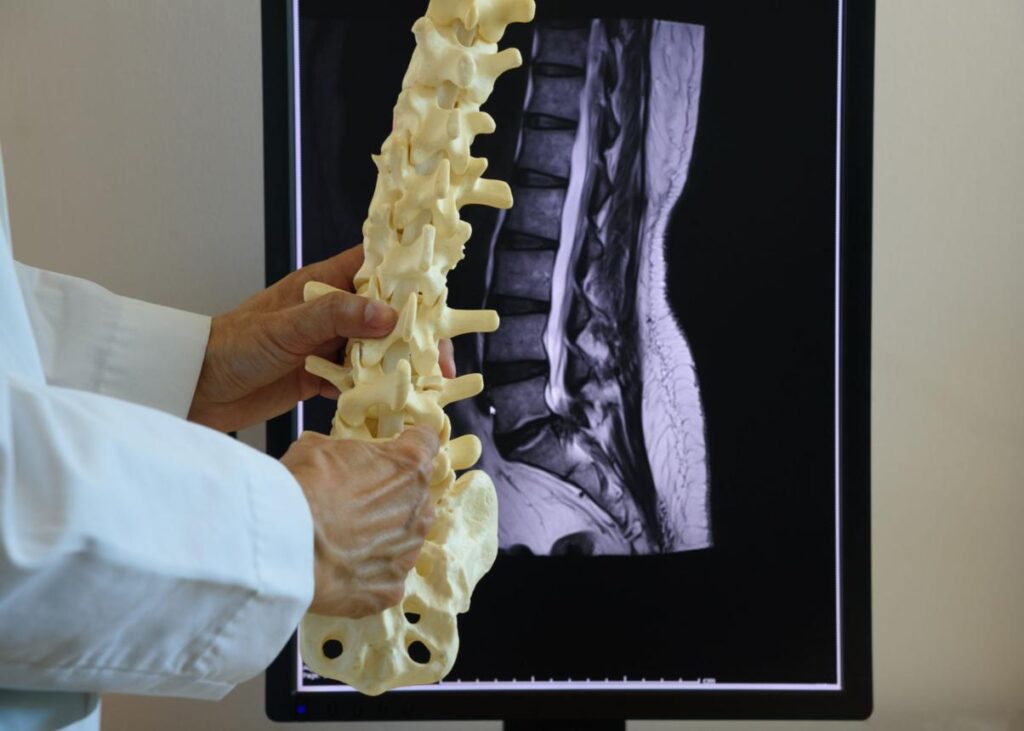
High-quality studies consistently show that microdiscectomy provides faster and more predictable relief of sciatica than continued non-surgical treatment.
In the SPORT trial, patients who underwent surgery experienced greater improvements in pain and function, with benefits remaining durable over long-term follow-up.
In a New England Journal of Medicine trial, patients with persistent sciatica had significantly less leg pain at 6 months after surgery, with average pain scores of 2.8 vs 5.2 (on a 0–10 scale) compared to non-surgical care.
The Peul randomized trial similarly showed faster relief and perceived recovery with early surgery, although many patients in the non-surgical group improved over time.
The overall takeaway is consistent. Many patients improve without surgery, but in the right patient, surgery offers faster and more reliable symptom relief.
References
Lumbar microdiscectomy has a strong long-term track record and remains the benchmark procedure for symptomatic disc herniation.
Prospective studies report clinically significant improvement in approximately 77% of patients for neurologic symptoms and 82% for pain and disability at 1 year.
Across the broader literature, success rates are generally reported in the range of 75–90% for meaningful improvement in leg pain and function.
Patients with shorter symptom duration tend to do better, while prolonged symptoms before surgery may be associated with slightly less improvement.
While the idea of a smaller incision is appealing, it’s important to look at the long-term trade-offs between “endoscopic” surgery and the traditional “microdiscectomy” performed with a microscope. Research shows that while endoscopic techniques use a smaller “keyhole,” they may carry a higher risk of nerve irritation. In fact, some studies found that 34.3% of endoscopic patients experienced temporary post-operative nerve sensitivity or “tingling” (dysesthesia), compared to only 3.3% of those who had a traditional microdiscectomy.


A lumbar microdiscectomy is a minimally invasive spine surgery that removes a portion of a herniated disc pressing on a nerve in the lower back. The goal is to relieve nerve compression and reduce leg pain (sciatica).
Patients with a herniated lumbar disc causing leg pain, numbness, or weakness that hasn’t improved with conservative treatments like physical therapy, medications, or injections may be candidates.
Lumbar microdiscectomy is most commonly used to treat sciatica, including leg pain, tingling, numbness, and weakness caused by nerve compression.
The procedure typically takes about 45 minutes to 1.5 hours, depending on the complexity of the case.
Yes, it is considered a minimally invasive procedure. It uses small incisions and specialized instruments to reduce muscle disruption and speed up recovery.
Most patients return to light activities within a few weeks and resume normal activities within 4–6 weeks, depending on their condition and job demands.
Many lumbar microdiscectomy procedures are performed on an outpatient basis, meaning patients can go home the same day.
As with any surgery, risks include infection, bleeding, nerve injury, or recurrence of the disc herniation, though complications are relatively uncommon.

The research supports a clear principle. Lumbar microdiscectomy works best when leg pain is clearly caused by a disc herniation that matches the patient’s symptoms, physical exam, and imaging findings.
For the right patient, most improve and many improve quickly. At the same time, some patients may continue to have symptoms, experience recurrence, or require additional treatment over time.
Microdiscectomy remains the reference procedure because of its consistent results, strong evidence base, and ability to directly address nerve compression.
When the diagnosis and treatment are aligned, it provides one of the most predictable paths to relieving sciatica.
References
1. Kreiner DS, Hwang SW, Easa JE, et al. An evidence-based clinical guideline for the
diagnosis and treatment of lumbar disc herniation with radiculopathy. Spine J.
2014;14(1):180-191.
2. Lurie JD, Tosteson TD, Tosteson ANA, et al. Surgical versus nonoperative treatment for
lumbar disc herniation: eight-year results for the Spine Patient Outcomes Research Trial
(SPORT). Spine. 2014;39(1):3-16.
3. Peul WC, van Houwelingen HC, van den Hout WB, et al. Surgery versus prolonged
conservative treatment for sciatica. N Engl J Med. 2007;356(22):2245-2256.
4. Bailey CS, Rasoulinejad P, Taylor D, et al. Surgery versus conservative care for persistent
sciatica lasting 4 to 12 months. N Engl J Med. 2020;382(12):1093-1102.
5. Gadjradj PS, Rubinstein SM, Peul WC, et al. Full endoscopic versus open discectomy for
sciatica: randomised controlled non-inferiority trial. BMJ. 2022;376:e065846.
6. Gadjradj PS, Harhangi BS, Amelink J, et al. Percutaneous transforaminal endoscopic
discectomy versus open microdiscectomy for lumbar disc herniation: a systematic review
and meta-analysis. Spine. 2021;46(8):538-549.
7. Bombieri FF, McVey J, Mikhail CM, et al. Complications associated with lumbar
discectomy surgical techniques: a systematic review. J Spine Surg. 2022;8(2):309-319.
8. Shriver MF, Xie JJ, Tye EY, et al. Lumbar microdiscectomy complication rates: a
systematic review and meta-analysis. Neurosurg Focus. 2015;39(4):E6.

