
From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

When patients are told they may need surgery for a lumbar disc herniation or sciatica, they often ask:
“What is the least invasive option?”
This often leads to a comparison between endoscopic spine surgery and microdiscectomy (also called microsurgical lumbar decompression).
Both are minimally invasive procedures, and both can be performed as outpatient spine surgery in appropriate cases. However, they differ in consistency, complication profile, versatility, and long-term reliability.
Current research shows that pain relief can be similar between the two procedures, but important differences remain when looking at nerve irritation, reoperation rates, and which patients are the best candidates.

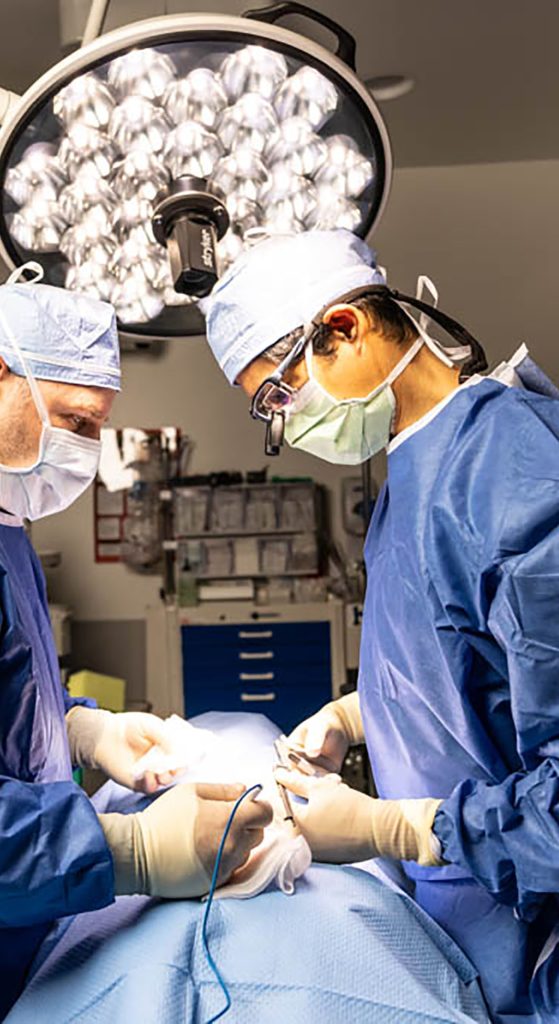
For most patients, the goal is not simply choosing the smallest incision. The goal is choosing the approach that provides the safest and most reliable outcome.
Key factors include:
Dr. Ronjon Paul focuses on evidence-based care and offers advanced options, including outpatient spine surgery, when appropriate, to help patients recover safely and effectively.

No. Current evidence shows similar outcomes between the two procedures, without consistent proof that endoscopic spine surgery is superior.
Microdiscectomy tends to have slightly lower or comparable long-term reoperation rates, depending on the study and patient selection.
Endoscopic spine surgery uses a small incision, but microdiscectomy is also minimally invasive. The difference is not always clinically meaningful.
Yes. In appropriate cases, microdiscectomy can be performed as outpatient spine surgery, allowing patients to return home the same day.
The best procedure depends on imaging findings, symptoms, anatomy, and overall health. A spine specialist can determine the most appropriate approach.

Endoscopic spine surgery continues to evolve, but current research does not show that it is consistently better than microdiscectomy.
For many patients with lumbar disc herniation or sciatica, microdiscectomy remains one of the most reliable and consistent surgical options.
When appropriate, Dr. Paul utilizes outpatient spine surgery techniques designed to reduce disruption, support recovery, and provide durable relief.
References
Systematic Reviews and Meta-Analyses (Highest Level Evidence)
Spine Surgery Yong JH, et al.
Full-endoscopic versus microscopic lumbar discectomy for lumbar disc herniation: A systematic review and meta-analysis of 4,186 cases. Spine Journal. 2026.
Patel T, et al. Comparative effectiveness of full-endoscopic versus micro-endoscopic and open discectomy: Systematic review and meta-analysis. Clinical Neurology and Neurosurgery. 2025.
Ruan W, et al. Percutaneous endoscopic lumbar discectomy versus open lumbar microdiscectomy: A meta-analysis.
International Journal of Surgery. 2016.
Cong L, et al. A meta-analysis of endoscopic discectomy versus open discectomy for lumbar disc herniation. Spine. 2016.
Muthu S, et al. Is endoscopic discectomy the next gold standard in lumbar disc surgery? A meta-analysis. Global Spine Journal. 2021.
Ravikumar S, et al. Comparative surgical approaches for lumbar disc herniation: Meta-analysis of outcomes. Journal of Spine Surgery. 2025.
Comparative Clinical Studies and Cohort Data
Masuda S, et al. Reoperation rates of microendoscopic discectomy compared with conventional microdiscectomy. Spine. 2023.
Lin CH, et al. Percutaneous endoscopic lumbar discectomy versus open discectomy: Comparative outcomes and recurrence rates. Tzu Chi Medical Journal. 2023.
Abudurexiti T, et al. Microendoscopic discectomy versus percutaneous endoscopic lumbar discectomy: Comparative effectiveness study. 2018.
Castel X, et al. Patient-reported outcomes following full-endoscopic lumbar discectomy. Spine Surgery and Related Research. 2025.
Complications, Dysesthesia, and Technical Considerations
Yang CC, et al. Complications of full-endoscopic lumbar discectomy: A systematic review.
Lewandrowski KU, et al. Dysesthesia due to irritation of the dorsal root ganglion following lumbar transforaminal endoscopy. Clinical Neurology and Neurosurgery. 2020.
Cembraneli PN, et al. Comparison between open microdiscectomy and endoscopic discectomy: A case series and literature review. Neurology & Neuroscience. 2025.
Technique Evolution, Indications, and Learning Curve
Kapetanakis S, et al. Full-endoscopic lumbar discectomy: A comprehensive review of techniques, outcomes, and indications. Journal of Clinical Medicine. 2025.
Di L, et al. Endoscopic lumbar microdiscectomy: Systematic review of preoperative characteristics and outcomes.
Maroun R, et al. Endoscopic discectomy for L4–L5 disc herniation: Meta-analysis comparing transforaminal and interlaminar approaches. Brain and Spine. 2026.

