
From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

From the first visit to full recovery, your care with Dr. Ronjon Paul is designed to be thoughtful, individualized, and transparent.
Proudly Affiliated with:

Anterior cervical discectomy and fusion (ACDF) and cervical disc replacement (CDR) are two of the most well-established surgical options for treating nerve or spinal cord compression in the neck.
Dr. Paul has over 20 years of experience performing both procedures and takes an individualized, evidence-based approach to each case. Because both options are routinely performed, recommendations are based on the patient’s anatomy, condition, and long-term goals — not on a single preferred technique.
Both procedures aim to relieve pressure on the nerves or spinal cord, improve function, and reduce pain. The key difference lies in how each approach handles motion at the affected level.

Both ACDF and cervical disc replacement are designed to remove pressure from the nerves or spinal cord, which is the primary cause of symptoms such as arm pain, numbness, weakness, and coordination issues.
In both procedures, the damaged disc is removed through an anterior approach in the front of the neck. This allows for direct access to the source of compression while minimizing disruption to surrounding structures.
The shared goal is consistent: relieve nerve pressure, restore alignment, and improve function. Where the procedures differ is in how they manage the spinal segment after decompression.
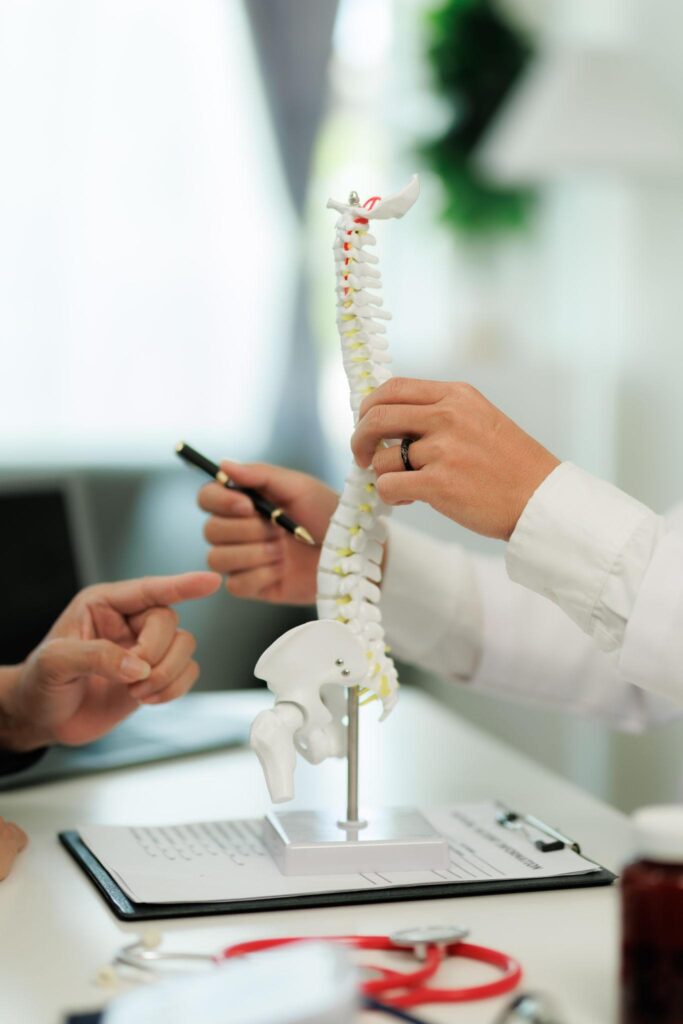
The primary difference between these procedures is how they treat motion at the affected level.
ACDF removes the damaged disc and stabilizes the spine by fusing two vertebrae into a single solid unit. This eliminates motion at that level but provides reliable stability, especially in cases of advanced degeneration or instability.
Cervical disc replacement removes the damaged disc and replaces it with a mechanical implant designed to preserve motion. This allows the spine to continue moving at that level, which may feel more natural for some patients.
Both approaches are effective. The decision depends on whether preserving motion or stabilizing the spine is more appropriate for the patient’s condition.
Both ACDF and cervical disc replacement provide excellent relief of arm pain and nerve-related symptoms in clinical studies.
Recovery timelines are generally similar, with both procedures allowing patients to return to activity over a predictable period.
One of the main differences is how the neck feels after surgery. Disc replacement preserves motion at the treated level and may feel more natural, while ACDF removes motion at that level. However, this difference is often less noticeable than expected.
By the time surgery is considered, many patients already have significantly reduced motion due to disc collapse and arthritis. In these cases, removing motion at a level that was already stiff often does not negatively affect overall function and may even improve comfort.
Long-term studies also show that disc replacement may lead to fewer adjacent-level surgeries compared to fusion in some patients over extended follow-up periods.
While cervical disc replacement offers the advantage of preserving motion, it also introduces implant-specific considerations.
Studies report revision rates for disc replacement in the range of 3–5%, with potential complications including implant migration, subsidence, and heterotopic ossification.
It is also important to understand that artificial discs do not fully replicate the complexity of a natural disc. While they restore movement, they do not reproduce the full biomechanics or shock-absorbing properties of a biological disc.
ACDF, on the other hand, eliminates motion at the treated level but has a long track record of predictable outcomes and remains the preferred option in cases of advanced degeneration, deformity, or multi-level disease.


ACDF removes the diseased disc and fuses the two vertebrae together, while cervical disc replacement removes the disc and places a mechanical implant designed to preserve motion at that level.
Cervical disc replacement preserves motion at the treated level. That said, many patients needing fusion already have severe arthritis and very little useful motion left at that level before surgery even begins.
Usually not as much as they fear. In many patients, the level being fused is already stiff from spondylosis and painful guarding. After decompression and pain relief, some patients actually feel they move better overall.
No. Artificial discs preserve functional motion, but they do not fully reproduce the complex shock absorption, viscoelasticity, and coupled motion of a natural cervical disc. They are helpful mechanical substitutes, not biologic duplicates.
Disc replacement introduces implant-specific risks such as migration, subsidence, heterotopic ossification, device wear, and more complex revision surgery if failure occurs. These problems are uncommon, but they are part of informed decision-making.
The best candidates often have one or two levels of soft disc disease, preserved facet joints, good alignment, and bone quality that supports an implant. It is generally a more selective operation than ACDF.
Patients with advanced spondylosis, collapsed disc spaces, major bone spur formation, deformity, instability, poor facet joints, or more extensive disease are often better served by a fusion for durable relief and stability.
Both have excellent long-term results when used in the right patient. Disc replacement may lower adjacent-level surgery rates in selected patients, while ACDF remains the time-tested standard for more advanced degeneration.
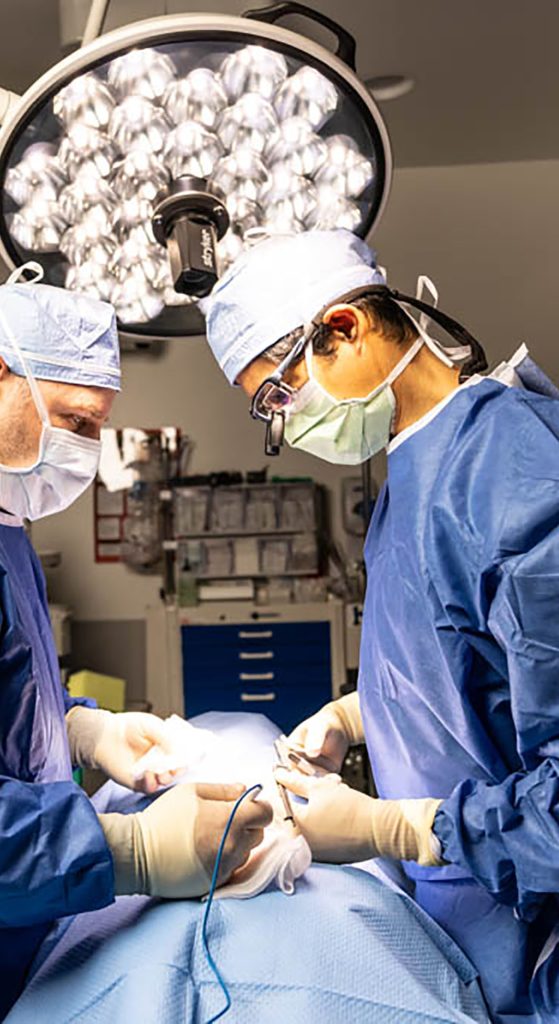
The research supports a clear principle. Both ACDF and cervical disc replacement are highly effective when used in the right clinical setting.
Disc replacement is often ideal for younger, active patients with preserved motion and limited levels of disease. ACDF is often preferred in patients with more advanced degeneration, instability, or multi-level involvement.
The most important factor is not the procedure itself, but how well it matches the patient’s anatomy, symptoms, and long-term goals.
Dr. Paul’s approach focuses on selecting the right operation for the right patient, ensuring that the treatment provides reliable, durable results while supporting long-term function and comfort.
References
1. Nunley PD et al. Mobi-C Cervical Disc: 10-Year Outcomes. Spine J. 2023.
2. Gornet MF et al. Prestige LP Cervical Disc 10-Year Data. Neurosurgery. 2022.
3. Wang F et al. Meta-Analysis: CDR vs ACDF Long-Term Results. Eur Spine J. 2019.
4. Chang SW et al. A Comparison of ACDF Versus TDR-C. Neurospine. 2018.
5. Shamji MF et al. Complications and Reoperations After Cervical Arthroplasty.
Neurosurgery. 2019.
6. Chen YS et al. Subsidence and Reoperation After CDR. Spine J. 2021.
7. Yi S et al. Heterotopic Ossification After CDR. J Neurosurg Spine. 2020.
8. Gornet MF et al. Revision Cervical Disc Arthroplasty: Mechanisms and Outcomes.
Spine. 2021.
9. Limanówka B et al. Changes in Cervical ROM Following ACDF. 2020.
10. Liang W et al. Biomechanical Adaptation After ACDF. Front Bioeng Biotech. 2022.
11. DiAngelo DJ et al. Biomechanics of Cervical Total Disc Replacement Compared with
Fusion. Spine. 2003.
12. Rousseau MA et al. Influence of Prosthesis Design on Kinematics. J Neurosurg Spine.
2008.
13. Puttlitz CM et al. Comparison of Artificial Disc Prostheses with the Natural Disc. J
Neurosurg Spine. 2004.
14. White AA III & Panjabi MM. Clinical Biomechanics of the Spine. 1990.

