About Lumbar Spondylolisthesis
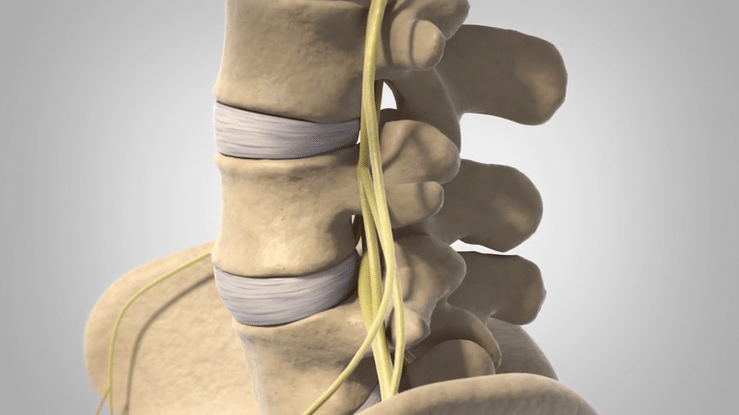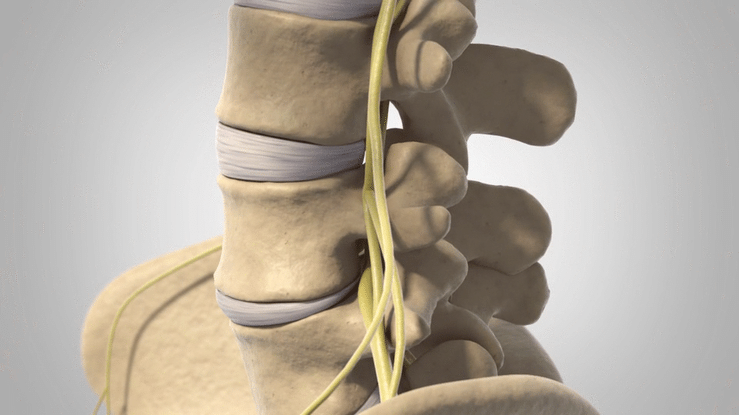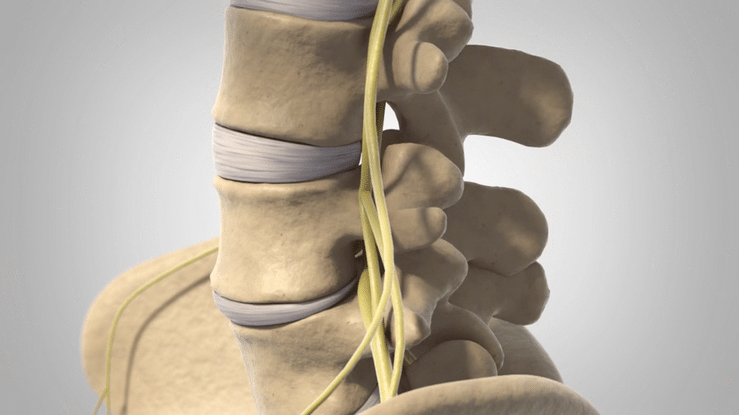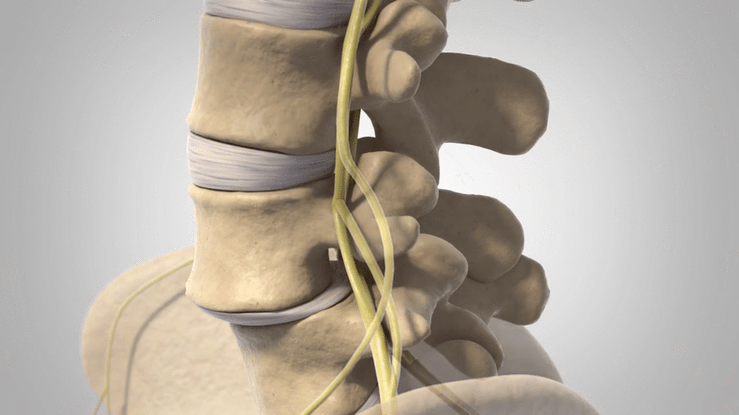
Lumbar Spondylolisthesis is characterized by instability in the vertebral column, most commonly in the region of the L4-L5 vertebrae. The origin of the name is Greek, with “spondy” referring to vertebrae and “listhesis” referring to movement.
Shifting vertebrae push on the spinal cord and can cause pain and numbness, especially when standing or bending over. Nonsurgical treatment options exist, and strengthening the muscles of the core can help compensate for the vertebral instability, but a number of more invasive procedures can be performed in more difficult cases.
About Lumbar Spondylolisthesis
Lumbar Spondylolisthesis is characterized by instability in the vertebral column, most commonly in the region of the L4-L5 vertebrae. The origin of the name is Greek, with “spondy” referring to vertebrae and “listhesis” referring to movement.
Shifting vertebrae push on the spinal cord and can cause pain and numbness, especially when standing or bending over. Nonsurgical treatment options exist, and strengthening the muscles of the core can help compensate for the vertebral instability, but a number of more invasive procedures can be performed in more difficult cases.
LOWER BACK AND/OR LEG PAIN
ABNORMAL POSTURE AND/OR A SHUFFLING GAIT WHEN WALKING
WEAKNESS IN THE LOWER EXTREMITIES
SCIATICA, AN ACHING PAIN IN THE HIPS, BUTTOCKS, AND LOWER BACK THAT RADIATES (SPREADS) INTO THE BACK OF THE THIGHS AND LEGS
How is Lumbar Spondylolisthesis managed?
Non-surgical management of lumbar spondylolisthesis will typically involve over the counter anti-inflammatory and analgesic medications such as NSAIDs, as well as physical therapy. Improving core strength has excellent effects on back pain, and lifestyle modifications may improve quality of life significantly. Steroid injections may also be performed to provide long term relief, however, are not recommended in patients for whom relief does not last for several months.
In patients unable to achieve satisfactory results with non-surgical options, decompression surgery with or without fusion will typically be performed. Decompression involves removing part of the bone and disc to improve the space within the spinal canal, and fusion may be necessary to then stabilize the vertebral column. Bone grafts are typically used to facilitate the fusion of vertebrae. These grafts may come from the patient themself, a cadaver donor, or a synthetic source depending on patient preference. Most patients will be up and walking the day after surgery, but three to six months are recommended before returning to all normal activities.

How is Lumbar Spondylolisthesis managed?
Non-surgical management of lumbar spondylolisthesis will typically involve over the counter anti-inflammatory and analgesic medications such as NSAIDs, as well as physical therapy. Improving core strength has excellent effects on back pain, and lifestyle modifications may improve quality of life significantly. Steroid injections may also be performed to provide long term relief, however, are not recommended in patients for whom relief does not last for several months.
In patients unable to achieve satisfactory results with non-surgical options, decompression surgery with or without fusion will typically be performed. Decompression involves removing part of the bone and disc to improve the space within the spinal canal, and fusion may be necessary to then stabilize the vertebral column. Bone grafts are typically used to facilitate the fusion of vertebrae. These grafts may come from the patient themself, a cadaver donor, or a synthetic source depending on patient preference. Most patients will be up and walking the day after surgery, but three to six months are recommended before returning to all normal activities.
How is Lumbar Spondylolisthesis diagnosed?
In less severe cases, physical examination and patient history are usually enough to make a tentative diagnosis. In more severe cases, however, imaging will often be necessary to evaluate the structures of the back, especially if considering surgery as an option. X-rays can provide rapid and clear visualization, but MRI and CT are sometimes ordered for a more detailed look into the nature of the condition for a given patient.
![dr ronjon paul md (1020x681px) - how is [condition] diagnosed? https://paulspine.com/wp-content/uploads/2021/01/dr-ronjon-paul-md-1020x681px-how-is-condition-diagnosed.jpg](https://paulspine.com/wp-content/uploads/2021/01/Dr-Ronjon-Paul-MD-1020x681px-How-is-condition-diagnosed.jpg)
![dr ronjon paul md (1020x681px) - how is [condition] diagnosed? https://paulspine.com/wp-content/uploads/2021/01/dr-ronjon-paul-md-1020x681px-how-is-condition-diagnosed.jpg](https://paulspine.com/wp-content/uploads/2021/01/Dr-Ronjon-Paul-MD-1020x681px-How-is-condition-diagnosed.jpg)
How is Lumbar Spondylolisthesis diagnosed?
In less severe cases, physical examination and patient history are usually enough to make a tentative diagnosis. In more severe cases, however, imaging will often be necessary to evaluate the structures of the back, especially if considering surgery as an option. X-rays can provide rapid and clear visualization, but MRI and CT are sometimes ordered for a more detailed look into the nature of the condition for a given patient.








